Vitamin D’s role in the human body
Despite its name, vitamin D is not a true vitamin; it is a pro-hormone. Vitamins need to be consumed from food because the body cannot produce them by itself. Vitamin D, on the other hand, can be synthesized by the body from sunlight, on top of dietary sources:
- Egg yolks -- Most of the protein is found in the egg whites, but the nutrients are found in the yolk. Compared to chickens that are raised indoors, pasture-raised or free-range chickens produce eggs that have higher amounts of vitamin D.
- Mushrooms -- They are the only plants capable of converting sunlight into vitamin D, making them the only plant source of this nutrient.
- Fatty fish and seafood -- Some examples of seafood rich in vitamin D are salmon, shrimp, and herring.
Vitamin D has a key role in multiple functions of the body. It helps maintain bone and teeth health, aside from regulating insulin levels and aiding in diabetes management.
Vitamin D is also important for the brain, immune system and nervous system. It regulates cell growth and cell-to-cell communication. In fact, some studies have suggested that calcitriol, an active form of vitamin D, can potentially inhibit cancer progression. (Related: Vitamin D Halts Growth of Breast Cancer Tumors.)
Vitamin D and the immune system
The list of research backing up vitamin D’s role in the immune system is long. In the Edinburgh study however, the researchers wanted to explore vitamin D’s influence on autoimmune diseases. Previous works have observed an inverse relationship between vitamin D and the susceptibility to autoimmune diseases. Some of these include Type 1 diabetes, multiple sclerosis, and rheumatoid arthritis.
In this study, the researchers took a closer look into how vitamin D affects two key cells in the immune system: dendritic cells and T cells.
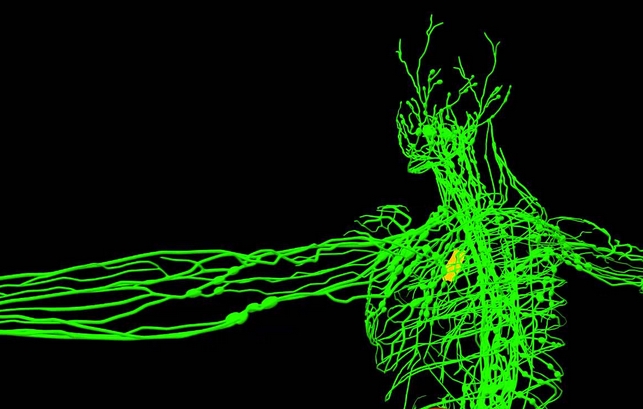
Dendritic cells are tree-shaped cells found in lymph nodes and the spleen. They regulate the immune system by capturing antigen cells and activating T cells. On the other hand, T cells are produced in the thymus, and they help fight infection. There are two kinds of T cells: Helper T cells, which aid other cells in the immune system; and cytotoxic T cells, which kill infected cells.
For people with autoimmune disease, this is not the case. When T cells become activated, they attack the body’s healthy tissues, not the aberrant ones. In this way, the body goes against itself, and the person has to take medications in order to maintain proper bodily functions.
The researchers collected cells from mice and humans and observed vitamin D’s reaction with them. The vitamin D caused dendritic cells to produce more of a certain molecule on their surface. This molecule was CD31. Its role as a part of the immune system has been unclear for the longest time. However, this study revealed that increased levels of CD31 inhibited the activation of T cells.
Acting as a barrier between dendritic cells and T cells, CD31 prevented the two from making stable contact. This resulted in a reduced immune reaction in the cell.
The researchers suggested that the study opens new doors for further exploring the roles of vitamin D and CD31 in the immune system. Managing the levels of vitamin D can potentially become a method to help control and maintain not only autoimmune diseases, but other ailments as well.
Sources include:
Please contact us for more information.