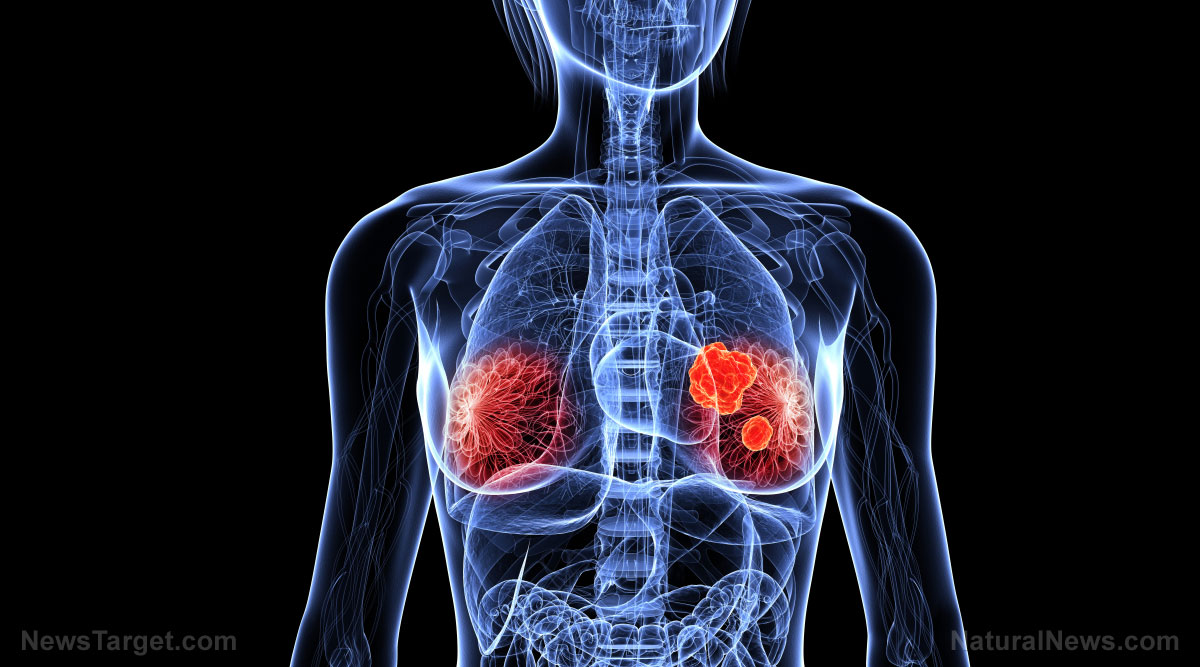
Published in the Science Immunology journal, the study is an exploration of possible methods to counter and eliminate cancer from the human body without harming healthy cells.
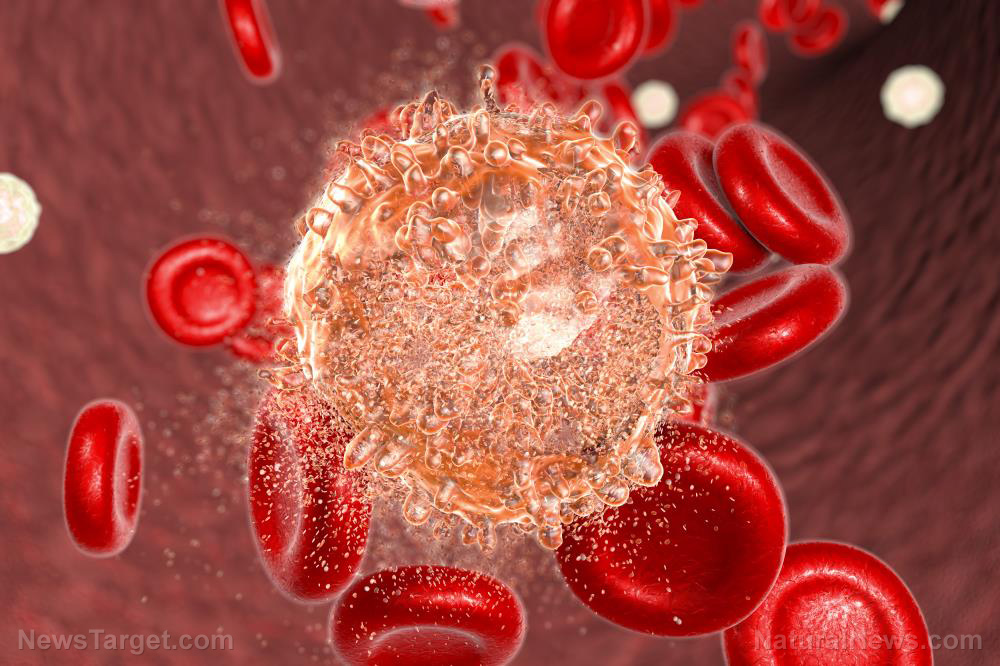
The study, conducted by researchers from the University of Washington, is hinged on the concept of necroptosis, a form of programmed cell death in which cells become riddled with holes, spurring them to release inflammatory chemical, which summon immune cells that subsequently kill off the damaged cells.
As detailed in the study, doctoral student Annelise Snyder and her colleagues first genetically engineered cancer cells that would turn necroptotic when activated. These cells were injected into melanoma or adenocarcinoma tumors that were grown on several lab mice.
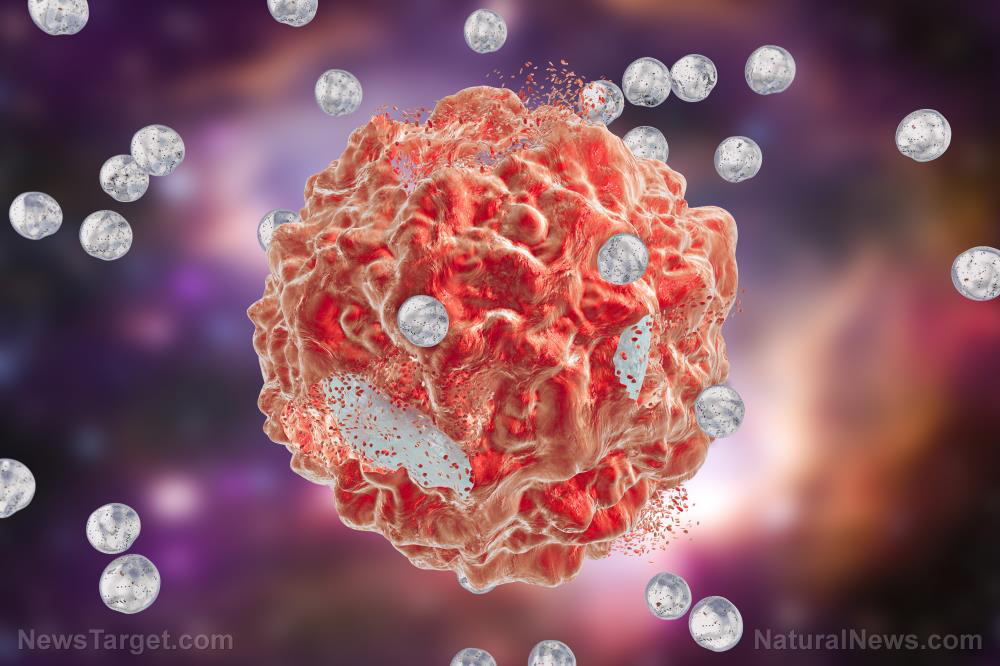
According to the researchers, they observed a significant decrease in the growth rate of the tumors – later revealed to be caused by the presence of killer T cells.
In addition to the slowing-down of the tumors, the dying, necroptotic cells spurred immune cells to attack cancer cells not just at the tumors, but throughout the bodies of the mice.
Furthermore, the animals injected with the necroptotic cells survived significantly longer than the mice that received injections of apoptotic cancer cells.
As detailed in the study, the necroptotic cells used in the first experiment were derived from the same cell line as the tumors, and therefore carried the same cell surface antigens. However, to the researchers’ surprise, they witnessed the same slowdown in terms of tumor growth when they injected necroptotic cells from a healthy fibroblast cell line into the tumors.
Senior author Andrew Oberst, a cancer immunologist at the University of Washington, said that their findings on necroptotic cells not having to carry any tumor antigen to have this effect was “surprising.”
According to Oberst, this suggests that the necroptotic cells don’t direct T cells to target tumors by displaying particular antigens, but rather by producing particular cytokines and chemokines that trigger the local T cells that reside around the tumor. As described in their research, these particular T cells are already primed to attack cancer cells, only needing an external “nudge” to become active – like throwing blood into the ocean to start a shark feeding frenzy.
“Location is everything,” Oberst said in their study. “Making this change to the tumor microenvironment by introducing necroptotic cells... is really what allows this to work.”
Additional experiments supported the importance of cytokines and chemokines in stimulating the immune system, according to the researchers. For instance, when they treated the necroptotic cells to curtail the production of those cytokines, and then injected them into tumors, they didn’t see the slowdown in growth they had observed in earlier experiments.
This was surprising, the researchers said, because it was long thought that necroptosis itself provoked the immune system.
“It’s not actually the death itself--the bursting of the cell, that is the key event,” Oberst said. “If we just induce cell lysis, we don’t see the same effect.”
Oberst added that triggering necroptosis is considered an attractive strategy over inducing apoptosis, because many tumors develop ways to block or evade the latter. However, Oberst clarified that many cancers and cancer cell lines such as breast cancer and acute myeloid leukemia develop necroptosis resistance. (Related: 9 Natural treatments for patients with breast cancer.)
According to Oberst, one way to circumvent this resistance may be via the viral delivery approach, wherein they engineer a virus that, once injected into melanoma tumors, would express similar tumor-controlling effects as the one they had observed in earlier experiments.
Oberst however, noted that they are still not sure if that method would have any “unwanted toxic effects.”
Oberst added that in the future, he and the rest of the researchers hope to experiment with tumor types that more closely resemble the cancers seen in humans.
For more information on cancer and cancer prevention, head over to PreventCancer.news.
Sources include:
Please contact us for more information.